What is colonic stenting?
Colonic stenting refers to the use of a self-expanding metallic cylindrical tube (stent) to keep the lumen of the large bowel open, not unlike coronary stenting where a stent is inserted to relieve blockage in the blood vessels of the heart. Colonic stenting is usually performed when there is complete or impending large bowel obstruction.
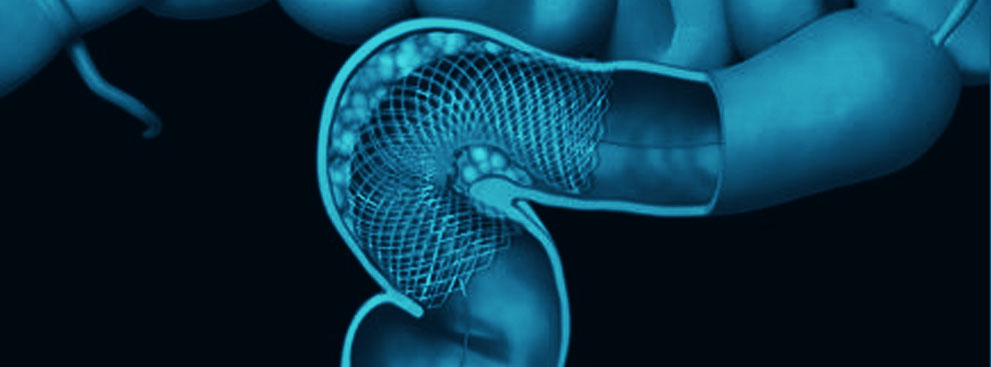
How is the colonic stent inserted and how does it work?
The stent is compressed in its closed form tightly into a small plastic delivery catheter. This allows the closed stent to be positioned across the tight narrowing in the colon causing the obstruction. The stent is inserted through a colonoscope, with the help of X-rays to identify the position of the stent. The stent is then opened by removing the plastic delivery catheter that keeps the stent compressed. Once opened, it relieves bowel obstruction by acting as a strut across the narrowed portion of the bowel.
In what situations are colonic stents used?
-
Colorectal Cancers causing bowel obstruction
Colonic stents are used to relieve bowel obstruction from colorectal cancers. Approximately 7-30% of colorectal cancer patients present with acute intestinal obstruction, when the cancer blocks up the lumen of the colon and does not allow the passage of stools past the cancer.
The traditional treatment of obstructed colorectal cancer is emergency surgery, which is usually performed via open surgery with a large abdominal wound, and is associated with a significant risk of complications and mortality, as well as a high chance of having a stoma.
Colonic stenting offers an alternative approach in the management of some patients with bowel obstruction from colorectal cancer. The stent temporarily opens up the lumen in the tumour, thus allowing stools to pass through and relieving the obstruction. Definitive surgery to remove the cancer, usually via a minimally invasive approach, is then performed a few weeks later.
The advantages of using the stent as a bridge to surgery (as compared with emergency open abdominal surgery) include:
- Lower rates of peri-operative complications
- Lower mortality rate
- Smaller wounds with less pain
- Lower chance of having a stoma
In a small group of patients, particularly those with advanced stage 4 cancer, the stent may be permanent. In these patients, the stent avoids the discomfort of a stoma and maintains the quality of life for a patient with terminal disease.
-
Benign strictures
Colonic stents are generally not recommended for the treatment of non-cancerous strictures in the colon. Theses may include strictures from diverticular disease, inflammatory bowel disease and radiation.
This is because the current colonic stents available on the market are not removable, which means that the stent is permanently in the colon and cannot be changed. The long term presence of a colonic stent can lead to stent complications such as stent erosion, stent perforation, stent migration, stent blockage and intra-abdominal abscess formation.
What are the risks of stenting?
The procedure is generally very safe and serious complications are not common. These may include:
- Failure to position the stent and having to abandon the procedure
- Bowel perforation
- Stent migration
Is colonic stenting a proven treatment for obstructed colorectal cancer? Does it affect long term cancer survival?
Studies have found colonic stenting to be an effective and safe method for treating acutely obstructed colorectal cancer, if the appropriate expertise is available. Although there were some initial concerns, recent studies have found that patients who have undergone colonic stenting followed by bowel resection surgery have good long term cancer survival outcomes.

