It may involve the bile ducts inside, outside the liver, or both. Choledochal
cysts occur more often in children, women and are more common in the Asian population.
Choledochal cyst is considered a potentially pre-cancerous condition, this risk of cancer
provides the basis for the current treatment strategies.
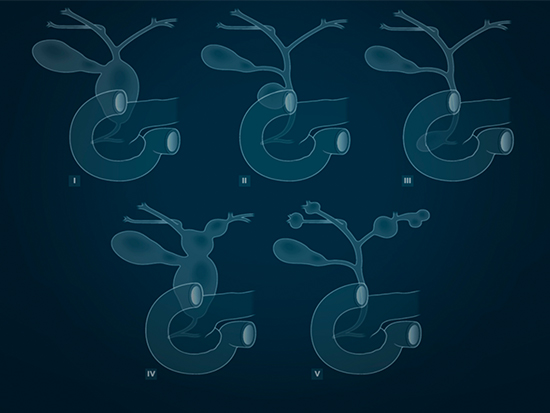
Cancer may develop in up to 20-30% of patients with choledochal cyst over time. Choledochal
cysts are classified according to their location and extent of involvement configurations.
Risk factors and Prevention
The exact cause is not known. It is a developmental abnormality of the bile duct which may be associated with other congenital anomalies. There is no known prevention but early diagnosis and treatment confers better outcomes.
What Are the Symptoms of Bile Duct Cysts?
- Some patients have no symptoms – these may be detected when scans are done for health screening or other conditions
- Obstructive jaundice - yellowing of the skin and eyes, itch, tea-coloured urine & pale stools
- Upper abdominal pain and discomfort- due to the cyst, an enlarged liver or associated pancreatitis (inflammation of the pancreas)
- Fever, chills & rigors- due to cholangitis (bacterial infection of the bile duct)
- Unexplained loss of weight and appetite
How Are Bile Duct Cysts Diagnosed?
The diagnosis of choledochal cyst is usually through imaging such as ultrasound. Other imaging tests such as CT, MRI/MRCP or ERCP may be necessary to further delineate the extent of the disease and guide surgical management.
Treatments for Bile Duct Cysts
Surgery is the best way to treat choledochal cyst. This involves surgical removal of the diseased
bile duct with the cyst and reconstructing the bile duct by joining the remnant bile duct to the
small intestine so as to re-establish the continuity of the digestive system.
If suitable, this can be approached via a minimally invasive “keyhole” techniques (laparoscopic, robotic) to minimise pain, scars, shorten hospital stay while optimizing recovery.
For more information, please consult our Hepato-Pancreato-Biliary (HPB) specialist.

