What is a hernia?
Hernias are protrusions of abdominal contents (fat or intestines) through a weakness in the abdominal wall (muscles and fascia) and present as a bulge or swelling. There are many types of hernias but the most common is the inguinal hernia at the groin area.
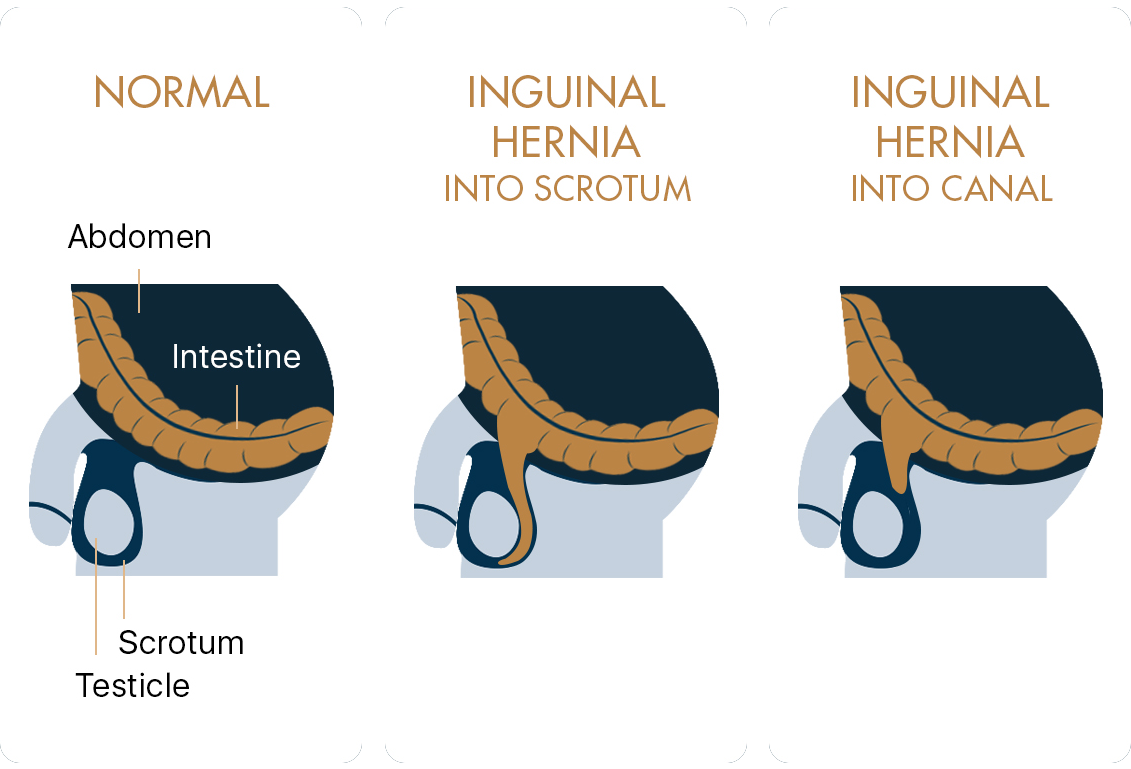
What are the causes of hernia?
Most hernias are caused by a combination of intra-abdominal pressure and an opening or weakness in the abdominal wall. The pressure pushes an organ or tissue through the opening or weak spot over time. Sometimes, muscle weakness is present at birth; more often, it occurs later in life.
Anything that causes an increase in pressure in the abdomen especially sudden or frequent increases in intra-abdominal pressure can cause a hernia, these include -
- Lifting heavy objects without stabilising the abdominal muscles
- Chronic constipation
- Persistent coughing or sneezing
- Weakness in the abdominal muscles/ fascia after surgery and/or contributed by poor healing
- Weakening of our muscles and fascia with age
- Obesity, poor nutrition and smoking can all weaken muscles and make hernias more likely
What are the signs and symptoms of hernia?
Hernias may become more apparent or bigger when the patient is standing or straining and it may disappear when lying down. It may also be associated with discomfort, a pulling or a heavy sensation and pain.
If left untreated, hernias may become irreducible and obstructed or strangulated. This happens when the blood supply to the contents of the hernia e.g. intestines, is cut off by the narrow opening of the hernia sac (neck). If left untreated, the patient will become very ill and the condition is potentially fatal as the intestines within can die.
When Should You Seek Treatment for a Hernia?
If you suspect a hernia or notice an unusual bulge, swelling, or pain, especially in the groin, consult our hernia surgeons for timely diagnosis and treatment.
How Is Hernia Diagnosed?
A hernia is typically diagnosed through a physical examination and a review of the patient's medical history. Common diagnostic methods include:
- Ultrasound – Creates images of the affected area using sound waves to visualise the hernia and determine its size and location.
- CT Scan – Provides detailed cross-sectional images of the body to identify hernias and evaluate any complications or associated conditions.
- Endoscopy – Uses a flexible tube with a light and camera to examine the upper digestive tract when a hiatal hernia is suspected.
- Barium Swallow – Involves ingesting a contrast material (barium) to highlight the oesophagus and stomach on X-rays for signs of abnormalities, including hiatal hernias.
What are the Treatments for Hernia?
Once a hernia forms, it will not heal by itself. Hernia surgery can be performed to repair a hernia and to prevent complications such as strangulation or obstruction from occurring.
Hernia surgery and treatment involve returning the abdominal contents to the abdominal cavity and reinforcing the weakened area of the abdominal wall. This is usually done with the insertion of a mesh over the weakened area. The mesh provides the scaffolding for the body to form strong scar tissue in the region where it is placed and strengthens the abdominal wall in that region. There are different types and sizes of mesh and your hernia surgeon will choose the best and most suitable one depending on the size and type of hernia you have.
Approaches
- Laparoscopic Approaches
- Traditional (Open)
Laparoscopic Hernia Surgery
Laparoscopic techniques can result in less pain and smaller scars and may be beneficial in
certain situations e.g. bilateral inguinal hernia, but not all hernias are suitable for
laparoscopic approaches.
Open approaches may still be recommended and may be better in certain situations where
laparoscopic approaches are not ideal e.g. large, chronic hernias.
The hernia repair treatment can be done under general anaesthesia, or under regional
anaesthesia.
Why Choose Us for Your Hernia Surgery in Singapore
At Surgical Associates, hernia care is delivered with attention to safety and individual needs. Speak to our surgeons about your hernia treatment options today.
What to Expect During Hernia Surgery
Hernia surgery is typically performed under general anaesthesia to ensure unconsciousness and comfort throughout the procedure. A small incision is made near the hernia site to access the affected area. The protruding tissue is repositioned, and the weakened muscle wall is reinforced using sutures, surgical mesh, or a combination of both. The incision is then closed with stitches, staples, or adhesive strips.
After surgery, the patient is monitored in a recovery area until stable. Pain and discomfort are common and are managed with prescribed medications and pain control strategies. The surgeon will provide detailed post-operative instructions on activity limitations, wound care, and follow-up appointments. Adhering to these instructions is crucial for optimal healing and minimising complications.
How Long Will It Take to Recover From a Hernia Surgery?
In fit, young patients with no significant medical problems, the hernia surgery can be performed as day surgery. Elderly patients or patients with more serious medical problems may require admission and may need to stay a day or two after surgery to recover.
After a hernia surgery, you may feel some numbness over the inner thigh (if surgery is performed for an inguinal hernia) and some tightness over the region of the surgery. This is due to the fibrosis and scarring that is taking place. This will mostly resolve over a few weeks.
You will be advised to refrain from carrying heavy loads and strenuous activities during the immediate postoperative period to allow healing to occur and to minimise recurrences, but you may gradually return to carrying loads and normal activities after a few weeks.
Potential Risks of Hernia Surgery
Hernia repair is generally a safe and effective procedure, especially when performed by an experienced surgical team. As with all surgeries, however, there are potential risks, including:
- Incision site infection
- Bruising or bleeding
- Temporary urinary retention
- Chronic pain
Rest assured that these risks are uncommon and steps are taken before, during, and after surgery to minimise them.
WHAT ARE THE COMMON TYPES OF HERNIAS?
Paraumbilical Hernias
Paraumbilical hernias are hernias that develop next to the belly button (umbilicus). They usually present as enlarging lumps or bulges that are more prominent when standing or straining. They can also become incarcerated and cause pain.
lncisional Hernias
Incisional hernias occur when the muscle and fascia layer underneath surgery scars become weak over time and/or contributed by poor healing e.g. wound infection. They can occur in various parts of the abdomen that have undergone abdominal surgery.
Femoral hernia
Femoral hernias occur when the intestine or fat enters the canal carrying the femoral vessels into the upper thigh, near the lower groin-inner thigh area. Femoral hernias are more common in women, especially in older, thin women.
FAQs About Hernia
Most hernias do not go away on their own and require surgery for effective treatment.
In some cases, small hernias without symptoms may not need immediate surgery. However, delaying increases complication risks like incarceration or strangulation. Consult a hernia specialist for personalised advice.
Incisional and femoral hernias tend to have a higher risk of recurrence than other types of hernias.
Follow your hernia doctor's post-operative instructions, especially on activity limitations and wound care. Maintain a healthy lifestyle through exercise, diet, and weight control. Employ proper lifting techniques and avoid unnecessary strain.
Men are more likely to develop inguinal hernias because of natural differences in their anatomy. In men, the inguinal canal is slightly weaker. This makes it easier for tissues or organs in the abdomen to push through and cause a hernia.
Prolonged sitting can worsen a hernia or increase the risk of developing one. If you have a hernia, it is important to be mindful of your activities and consult a doctor for appropriate advice and treatment.
Our Hernia Specialists in Singapore

Senior Consultant Hepatopancreatobiliary Surgeon
MBBS, MMed (Surgery), MSc, FAMS, FRCSEd
Dr Lee Ser Yee is a dual USA fellowship-trained hernia surgeon in Singapore, recognised for his expertise in minimally invasive and complex abdominal surgery. Formerly a Senior Consultant and founding member of the HPB and Transplant Surgery Department at SGH, he also led advanced laparoscopic and surgical skills training programs. Dr Lee takes a comprehensive approach to hernia repair, backed by deep experience in treating a wide range of abdominal conditions, including those requiring intricate surgical care.

Senior Consultant Colorectal Surgeon
MBBS, MMed (Surgery), FAMS, FRCSEd
Dr Tan Wah Siew was among the first female surgeons in Singapore trained in robotic colorectal surgery. She served as a senior consultant surgeon at the Department of Colorectal Surgery at SGH before moving into private practice. While she specialises in complex colorectal conditions, Dr Tan also has extensive experience in hernia repair and other abdominal surgeries. Her broad surgical expertise ensures patients receive thorough, personalised care tailored to their hernia and abdominal health needs.

